How To Repair A Mitral Valve
- Enquiry article
- Open Admission
- Published:
Mitral valve repair, how to make book not thing; techniques, tendencies, and outcomes, a single center experience
Periodical of Cardiothoracic Surgery book 13, Article number:108 (2018) Cite this article
Abstract
Background
Contempo evidence has showed u.s. that quality of mitral valve repair is strongly related to volume. Nonetheless, this study shows how depression-volume centers can achieve results in mitral valve repair surgery comparable to those reported past referral centers. It compares outcomes of mitral valve repair using resection versus noresection techniques, tendencies, and rates of repair.
Methods
Between 2004 and 2017, 200 patients underwent mitral valve repair for degenerative mitral valve disease at Fundación Cardioinfantil-Institute of Cardiology. L-eight (29%) patients underwent resection and 142 (71%) noresection.
Results
Follow-up was 94% complete, mean follow-upwards time was 2.3 years. There was no 30-day mortality. Five patients required mitral valve replacement after an average of 5.three years (Resection = 2; Noresection = 3). Freedom from severe mitral regurgitation was 98% at 6.6 years of follow-up for the noresection group, and 92.5% at 7 years for the resection group (log rank: 0.888). At last follow-upward, ii patients died of cardiovascular disease related to mitral valve, 181 patients (86%) showed no or grade I mitral regurgitation. Patients with previous myocardial infarction had increased take a chance of recurrent mitral regurgitation (p = 0,030). Within four years, we inverted the proportion of mitral valve replacement and repair, and in 2016 we accomplished a mitral valve repair rate of 96%.
Decision
This report suggests that resection and noresection techniques are safe and effective. Recurrence of astringent mitral regurgitation and need for mitral valve replacement are rare. We show that low-book centers can achieve results comparable to those reported worldwide by establishing a mitral valve repair team. We encourage hospitals to follow this model of mitral valve repair program to decrease the proportion of mitral valve replacement, while increasing mitral valve repair.
Groundwork
Mitral valve repair (MVr) is the aureate standard for the handling of mitral regurgitation (MR) secondary to degenerative mitral valve (MV) disease. MVr was initially performed past Alain Carpentier in 1983, who adult a standardized approach to correct MR, dubbed "the French correction". It involved leaflet resection followed past annular plication with or without sliding plasty in social club to restore the coaptation surface [1]. Excellent, reproducible results led to this technique becoming the gold standard to treat mitral valve prolapse. In 1998, Tirone David et al. proposed a novel repair technique using extended polytetrafluoroethylene (ePTFE) sutures for chordal replacement, preserving leaflet tissue and improving surface of coaptation [ii].
Subsequent studies accept shown splendid results for both techniques in terms of mortality, morbidity, and liberty from recurrent MR [iii]. Controversy remains as to which technique is superior given lack of long-term follow-up with creation of neochordae and the perception that this technique is more than difficutl to standardize, preventing widespread application.
In Latin America, long-term results of MVr remain unknown and the established practise is to supercede rather than repair the MV. The nowadays study was carried out to evaluate the short and long-term results of MVr using resection (R) versus noresection (NR) techniques in a low-volume center and resolve if a depression-volume center tin attain MVr results comparable to those reported worldwide. We analyzed freedom from reoperation, recurrent MR, and functional condition, as well as the change in the tendency of MVr and mitral valve replacement (MVR) at our institution over the study period. The findings of the study seek to improve cardiac surgery.
Methods
Patients
From Jan of 2004 to June 2017, 200 patients underwent MVr due to degenerative MV disease at Fundación Cardioinfantil- Institute of Cardiology, in Bogotá Colombia. Patients were identified through an institutional cardiac surgery database. Operational definitions, demographic variables, preoperative, intraoperative characteristics, and thirty-day outcomes were obtained retrospectively co-ordinate to the Order of Thoracic Surgeons database guidelines [4].
50-8 patients (29%) were in the R grouping and 142 (71%) in the NR group (chordal replacement or just ring annuloplasty). Twelve patients (6%) were lost to follow up.
Interventions
Operations were performed through a conventional median sternotomy or minimally invasive techniques (correct lateral minithoracotomy or periareolar approach). In the conventional arroyo, cardiopulmonary bypass was established through standard bicaval and aortic cannulation with moderate hypothermia. Intraoperative transesophageal echocardiography was used routinely in all patients. Access to the MV was performed through a left atriotomy. Next, segmental analysis of the MV was performed as described by Carpentier and colleagues [5]. In all patients, ring annuloplasty was performed with a semi-rigid, complete ring Fig. 1.
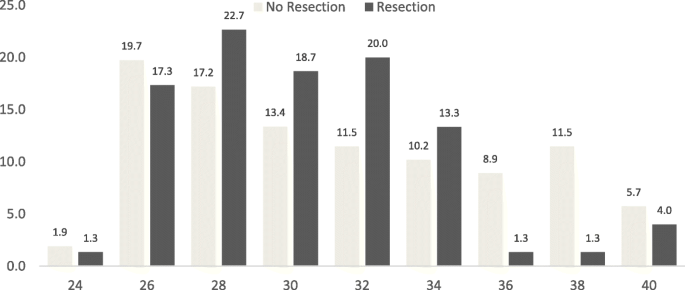
Size of annuloplasty ring. The figure shows the size of annuloplasty band past resection group. Size of the band is depicted on de y-centrality and the percentage on the x-axis
When the repair was performed minimally invasively, the femoral vessels were cannulated using modified Seldinger technique under echocardiographic guidance. A Chitwood clamp was used and cardiac abort achieved using HTK or Del Nido cardioplegia. Video help was used routinely.
Chordal replacement was performed with 5.0 ePTFE sutures without pledgets, passed as a figure of eight through the tip of the papillary muscle, followed past a figure of eight through the free edge of the prolapsing segment. A minimum of 2 neochordae were placed, and sutures were added depending on the size of the prolapsing segment. The height of the neochordae was established by filling the ventricle with a cold cardioplegic solution to examination the valve hydrostatically. The number of neochordae ranged from one to seven pairs (hateful: ane.88). A single pair of neochordae was used in 29% and multiple in 71%. The decision to perform either a R or NR technique was left to the surgeon's criteria.
Surgical data were obtained by systematic chart review, emphasizing the MVr technique and approach.
Information collection
Preoperative (age, previous cardiac operation, functional class, Euroscore II, left ventricular ejection fraction, previous arrhythmia, and medical history) and postoperative variables (length of stay, cross-clamp and cardiopulmonary bypass time, reoperation for bleeding and thirty-mean solar day mortality) were described.
Follow up was performed by telephone or in person (clinic visits). Endpoints were recurrent MR, reoperation or death. Echocardiographic evaluations were performed postoperatively before discharge, 30 to 90 days after surgery, then annually thereafter. The severity of MR was classified as none/petty (0), balmy (I), moderate (II) or severe (Iii). New York Heart Association (NYHA) functional grade was assessed in all the patients. Echocardiographic data were used for analysis but if at that place were at to the lowest degree two echocardiographic reports bachelor.
We described tendencies and number of cases of MVR and MVr for degenerative MV illness from 2004 to 2016. Data were obtained from the institutional cardiac surgery database.
Statistical assay
Baseline demographics and clinical characteristics were summarized using descriptive statistics. For continuous variables, information were presented as mean or median and standard deviations or interquartile range. Chiselled variables were presented as accented numbers and percentages. The frequency of MR was described. The divergence between the groups R and NR were ascertained using chi-square test or Fisher test, and Mann-Whitney U exam. The endpoint of interest was recurrent severe MR, MV reoperation or death. Patients that did non achieve the endpoint were censored at the end of study time. Survival was analyzed through Kaplan-Meier method; the log-rank exam was used to determine differences between groups. Statistical analysis was done with Stata SE xiv (program). A significance level of 0.05 was used throughout the analysis.
Results
Demographic data
Follow-up was 94% complete with a mean fourth dimension of 2.33 years. Preoperative variables are summarized in Table one. Of all patients, 122(61%) were male, and the average historic period at operation was 58 (48–58) years for the NR group and 56 (50–65) years for the R group. Before surgery, NYHA functional class was assessed in all the patients, 21 (x.5%) were in NYHA class I, 135 (67,v%) class II and 33 (xvi,5%) class 3. Iii (1.five%) patients had a history of myocardial infarction before surgery, all of them belong to the NR group. We establish differences in the left ventricular ejection fraction (LVEF) between groups; 55% (50–60%) and 60% (51–65) for the NR group and R group, respectively (p = 0.013).
Euroscore II was calculated in all patients earlier surgery. 50.iv% in the NR group were classified as low risk, compared to 25,9% in the R group (run a risk < ii%) Fig. 2.
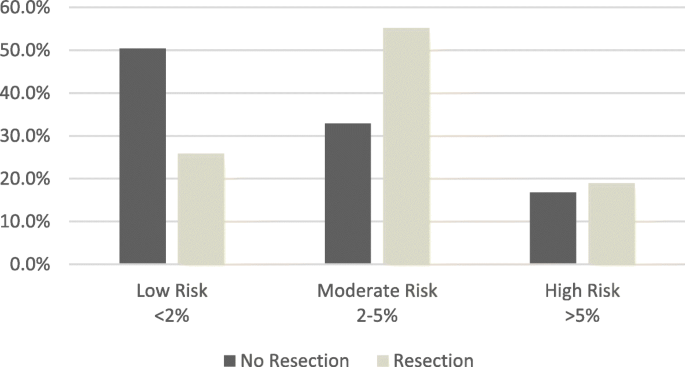
Preoperative Euroscore Two risk assessment. Figure shows Euroscore Two risk cess in NR and R groups
Perioperative outcomes
Perioperative variables are summarized in Tabular array ane. One hundred and seven patients (75%) of the NR group and 48 (84.v%) of the R grouping underwent isolated MVr. Mean cardiopulmonary bypass time was similar for both groups, 117 min (IQR 95–141) and 117 min (IQR 105–143) for the NR and R groups respectively. Forty-seven (33.one%) patients from NR group and 35 (60%) from R group had a posterior leaflet prolapse (p = 0,004). There was a statistically significant deviation in the number of minimally invasive procedures performed in each group, with 51 (32.nine%) in the NR group and seven (12.1%) in the R group (p = 0.001). Overall thirty-day bloodshed was 0%.
Survival outcomes
NYHA class and incidence of MR at last follow-upwards in 188 patients are reported in Table 2. Functional class was assessed in all the patients, most of whom showed significant comeback: 156 (83%) had NYHA class I, 25 (thirteen%) grade II, 5 (3%) class III and 2 (ane%) class 4. Patients in NYHA class Four had concomitant chronic obstructive pulmonary disease (COPD). Ninety-eight patients (52%) had none/trace MR, mild MR in 70 (37%), and moderate/astringent in 20 (10%).
There were only two cardiac-related deaths at last follow-upwardly. Liberty for severe MR was 98% at 6.6 years of follow-up for the NR grouping, and 92.5% at 7 years of follow-upwards for the R grouping. Based on MVr technique, patients in the R grouping had the same likelihood of developing MR compared to patients in NR group (log rank: 0.881). Five patients required an MV replacement later on an boilerplate of five.three years, 3 belonged to the NR group and 2 to the R grouping Fig. iii.
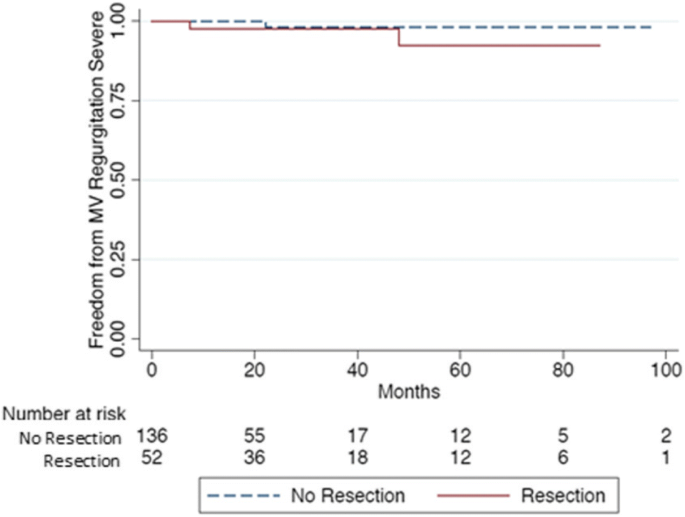
Freedom from > 3 Mitral Regurgitation. Kaplan-Meier gauge of survival function from at least > 3 mitral valve regurgitation for 188 patients with degenerative mitral valve illness
Bivariate analysis
In the bivariate assay, patients with previous myocardial infarction had an increased risk of developing at least moderate recurrent MR (p = 0,030). Preoperative variables such as diabetes, dialysis, dyslipidemia, hypertension and previous arrhythmia, were not associated with an increased adventure of developing recurrent MR afterward MVr. Patients that underwent minimally invasive repair, had a lower risk of developing recurrent MR (p = 0,040) Table 3.
Mitral valve surgery tendencies and repair rate
Tendencies and number of cases of MVr and MVR for degenerative MV illness are shown in Fig. four. Within iv years, we inverted the tendency and were able to maintain MVr every bit preferred technique of MV intervention. The MVr rates at our institution are shown in Fig. 5. Over the years there has been a constant increase in MVr rate, achieving a 96% repair charge per unit in 2016.
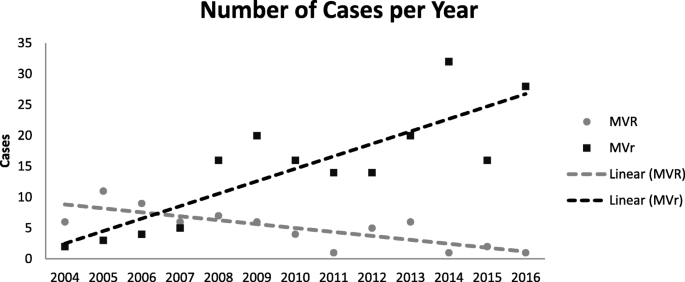
Trends and Number of Cases of Mitral Valve Repair and Replacement. Tendencies and number of cases for degenerative mitral valve repair and replacement betwixt 2004 and 2016. MVr: Mitral Valve Repair MVR: Mitral Valve Replacement
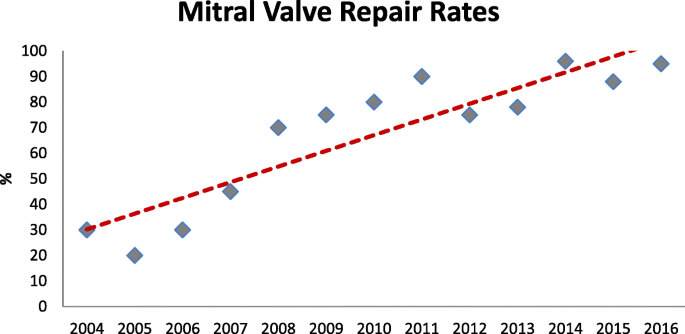
Mitral Valve Repair Rate. The effigy shows mitral valve repair rates over the years, tendency line is shown in ruby
Give-and-take
MV regurgitation is frequently caused by degenerative MV disease leading to myxomatous changes with chordal elongation with or without rupture [six,7,eight]. R and NR techniques accept shown excellent results, with low incidence of progression to severe MR and demand for MVR [7,viii,ix]. In our serial, five patients required MVR afterward an average of 5.iii years, three belonged to the NR group and two to the R grouping, one patient from the NR group had an ePTFE chord rupture. Schwartz et al. [x] described like results with a freedom from reoperation of 89% at ten years. There was no 30-day mortality in our series; Lange et al. [11] showed comparable results with 30-twenty-four hours mortality of 1%. We were able to achieve MVr results with R and NR techniques similar to those reported past referral institutions, despite being a low-volume center.
NR techniques, like chordal replacement, preserve leaflet mobility increasing coaptation surface and avoiding outflow tract obstruction. How to standardize length of the neochordae and the long-term durability of the reapir remain subjects of debate [eleven, 12]. In our series survival rates of NR techniques for severe MR were 77% (CI 95% 0.38–0.93) at 6.six years of follow-up and liberty from reoperation was 98.40%. Salvador et al. [13] reported 608 consecutive MVr with NR techniques, with a liberty from reoperation of 92% afterwards 15 years.
R techniques take exhibited excellent results [1, 11], yet, these techniques sometimes cede a large amount of valve tissue, resulting in leaflet brake, and requires a skilled and experienced surgeon. New techniques, similar butterfly resection, have been shown to preclude systolic anterior move, decreasing the need for annular plication [14, 15]. In our serial survival rates of R techniques for astringent MR were 92.4% (CI 95% 0.69–0.98) at 8.three years of follow-up, with a freedom from reoperation of 96%. Sakamoto et al. [sixteen] reported the long-term results of this techniques, with a liberty from reoperation of 92,3% at ten years.
In the matter of functional class, the results are excellent; the majority of patients showed considerable comeback after surgery. In our series, at terminal follow-up, 156 (82,9%) were in NYHA class I and 181 patients (86%) showed no or course I MR, with no difference between groups. Lange et al. [11] described similar results, at concluding follow-up 94% of their patients showed no or grade I MR. The literature supports that the incidence of severe MR, need for reoperation, and death are as low with R and NR techniques [11, 17,18,19,20,21]. However, the institutions were these investigations were conducted had high-volumes of MVr. It was uncertain if centers with low-volume could reproduce these results.
In our bivariate analysis, we found that patients that underwent minimally invasive repair had a lower hazard of developing recurrent moderate MR. This could exist explained by the fact that in our exercise, minimally invasive MVr is performed by a single surgeon (JPU), who too has the most feel. Further analysis has also shown, that minimally invasive MVr has resulted in earlier referral of patients by cardiologists, leading to patients being healthier, with less comorbidities. Since the NR group had more than minimally invasive repairs, this could explain the departure in euroscore 2 assessments between groups.
Our results show that, despite low volumes in the before years of our feel, MVr results accomplished can be comparable to those reported by referral centers worldwide, leading to an inversion in the trend of MVR vs MVr in our Institution and an excellent MVr rates. We aspect this change to the creation of a MVr program, with a dedicated squad lead by a MV surgeon (JPU) resulting in better patient option, standardization of processes and procedures, instruction of referring physicians, earlier patient referral, and better postoperative care and follow-up.
To improve volume and results of the MVr plan, we began to encourage targeted referral and guideline-based assessment of MV pathology. Cardiology, imaging, and disquisitional intendance teams were optimally equipped and physicians were trained so an earlier referral could be achieved. All MV cases were analyzed by the MVr plan before the procedure, and the repair was performed by an experienced surgeon. Cardiac anesthesiologists in charge of the cases were fully prepared to perform echocardiograms in the operating room so the quality of the MVr could be assessed earlier the patient was weaned of CPB. Junior cardiac surgeons were mentored and technically supported. A valvular heart clinic was created then MV patients could be properly followed and controlled.
With target and earlier referral, we improved patient option and MVr rates. We were able to operate healthier patients, with less comorbidities, meliorate functional course, younger, and with ameliorate LVEF. This was a cardinal gene for achieving and maintaining adept results, since patients with previous myocardial infarction, dyslipidemia, dialysis, and hypertension have an increased risk of developing at least moderate recurrent MR, as shown before in different studies [20,21,22,23]. The literature has suggested a close relationship between preoperative comorbidities and the odds of developing recurrent MR. Fukuda et al. [24] plant a close relationship between type 2 diabetes and the progression of MR. Nosotros performed an exploratory logistic binary regression, finding that previous myocardial infarction past itself increases the take a chance up to eighteen% and tin exist modified in the presence of variables such as age, gender, and surgical arroyo.
Different articles [25, 26] have shown that private surgeon volume is a determinant of MVr rates, liberty from reoperation, and survival. A total of < 25 MVr per year has been associated with poor results and depression MVr rates. When no book-outcome relationships were available, the United kingdom proposed a volume threshold of 25 MVr/year for surgeon, then better results could exist achieved. In the United states, there is no minimum volume standardized for MVr [26]. At our establishment, since the creation of the MVr programme, patient volume has grown and MVr rate has improved. Nosotros accept been able to maintain MVr as preferred technique of MV intervention, and satisfactory results have been obtained. With the creation of a well prepared, well equipped and experienced MVr program, that has a guideline-cess of MV pathology and is lead by an experienced MV surgeon, adequate MVr results can be accomplished in low-volume centers.
Daneshmand et al. [25] conducted a 20-twelvemonth study, and concluded that MVr patients have better survival and functional outcomes, especially after 10–15 years, compared to MVR. In keeping with this, Gammie et al. [27] presented the trends of MV surgery in the United States, showing progressive adoption of MVr. In Latin America, nonetheless, trends of MV surgery remain unknown, with piddling data showing trends in MVr vs MVR and unlike studies have suggested the number of MVr should be increased [27].
This paper has some limitations, it was a retrospective study performed over a menses of 15 years. Changes in surgical techniques and postoperative management of the patients might accept affected the incidence of recurrent MR.
Conclusions
In conclusion, short and long-term results with either the R or the NR techniques are equivalent. Recurrence of severe MR and the demand for MVR are rare. Significant symptomatic improvement can be achieved in more than 80% of the patients, and the majority will nowadays with no or grade I MR. Risk factors for MR after surgery should exist analyzed. The most reliable and durable repair technique for degenerative MV illness is the ane that the surgeon feels more comfortable and has the most experience with. This report shows how low-volume centers can achieve results comparable to those reported worldwide as recently suggested past Bakaeen et al. [28]. We attribute the results presented in this paper to the cosmos of a MVr team, with a dedicated MVr surgeon every bit the leader.
Abbreviations
- ePTFE:
-
Polytetrafluoroethylene
- MR:
-
Mitral regurgitation
- MV:
-
Mitral valve
- MVr:
-
Mitral valve repair
- MVR:
-
Mitral valve replacement
- NR:
-
No resection
- NYHA:
-
New York Centre Clan
- R:
-
Resection
References
-
Carpentier A. Cardiac valve surgery--the "French correction". J Thorac Cardiovasc Surg. 1983;86(3):323–37.
-
Perier P, Hohenberger W, Lakew F, Batz K, Urbanski P, Zacher M, et al. Toward a new paradigm for the reconstruction of posterior leaflet prolapse: midterm results of the "respect rather than resect" approach. Ann Thorac Surg. 2008;86(iii):718 -25-25.
-
Perier P, Hohenberger W, Lakew F, Diegeler A. Prolapse of the posterior leaflet: resect or respect. Ann Cardiothorac Surg. 2015;iv(3):273–seven.
-
Society of Thoracic Surgeons [Internet] . [cited 2017 Oct x]. Available from: https://www.sts.org/registries-inquiry-center/sts-national-database/developed-cardiac-surgery-database/data-collection. Accessed 07 Oct 2017.
-
Carpentier AF, Lessana A, Relland JYM, Belli E, Mihaileanu S, Berrebi AJ, et al. The "physio-band": an advanced concept in mitral valve annuloplasty. Ann Thorac Surg. 1995;threescore(v):1177–86.
-
Davies MJ, Moore BP, Braimbridge MV. The floppy mitral valve. Study of incidence, pathology, and complications in surgical, necropsy, and forensic material. Br Middle J. 1978;twoscore(5):468–81.
-
Sawazaki M, Tomari S, Zaikokuji K, Imaeda Y. Controversy in mitral valve repair, resection or chordal replacement? Gen Thorac Cardiovasc Surg. 2014;62(10):581–5.
-
Tomita Y, Yasui H, Iwai T, Nishida T, Morita S, Masuda M, et al. Extensive use of polytetrafluoroethylene artificial grafts for prolapse of posterior mitral leaflet. Ann Thorac Surg. 2004;78(3):815–9.
-
Deloche A, Jebara VA, Relland JY, Chauvaud S, Fabiani JN, Perier P, et al. Valve repair with Carpentier techniques. The 2d decade. J Thorac Cardiovasc Surg. 1990;99(half dozen):990–1001-ii.
-
Schwartz CF, Grossi EA, Ribakove GH, Ursomanno P, Mirabella Yard, Crooke GA, et al. Ten-yr results of folding Plasty in mitral valve repair. Ann Thorac Surg. 2010;89(two):485–8.
-
Lange R, Guenther T, Noebauer C, Kiefer B, Eichinger W, Voss B, et al. Chordal replacement versus quadrangular resection for repair of isolated posterior mitral leaflet prolapse. Ann Thorac Surg. 2010;89(4):1163–lxx.
-
Kobayashi J, Sasako Y, Bando Grand, Minatoya K, Niwaya 1000, Kitamura Due south. Ten-yr experience of chordal replacement with expanded polytetrafluoroethylene in mitral valve repair. Circulation. 2000;102(nineteen Suppl 3):III30–4.
-
Salvador 50, Mirone Due south, Bianchini R, Regesta T, Patelli F, Minniti G, et al. A 20-year experience with mitral valve repair with artificial chordae in 608 patients. J Thorac Cardiovasc Surg. 2008;135(6):1280–7.
-
Jebara VA, Mihaileanu Southward, Acar C, Brizard C, Grare P, Latremouille C, et al. Left ventricular outflow tract obstacle after mitral valve repair. Results of the sliding leaflet technique. Apportionment. 1993;88(5 Pt 2):II30–4.
-
Grossi EA, Galloway AC, Kallenbach K, Miller JS, Esposito R, Schwartz DS, et al. Early results of posterior leaflet folding plasty for mitral valve reconstruction. Ann Thorac Surg. 1998;65(4):1057–9.
-
Sakamoto Y, Hashimoto Grand, Okuyama H, Ishii S, Kawada North, Inoue T, et al. Mitral valve reconstruction: long-term results of triangular resection for degenerative prolapse. Gen Thorac Cardiovasc Surg. 2008;56(ii):63–7.
-
David TE, Omran A, Armstrong S, Dominicus Z, Ivanov J. Long-term results of mitral valve repair for myxomatous affliction with and without chordal replacement with expanded polytetrafluoroethylene sutures. J Thorac Cardiovasc Surg. 1998;115(six):1279–85.
-
Falk V, Seeburger J, Czesla M, Borger MA, Willige J, Kuntze T, et al. How does the utilize of polytetrafluoroethylene neochordae for posterior mitral valve prolapse (loop technique) compare with leaflet resection? A prospective randomized trial. J Thorac Cardiovasc Surg. 2008;136(5):1205–6.
-
Dogan South, Aybek T, Risteski PS, Detho F, Rapp A, Wimmer-Greinecker G, et al. Minimally invasive port access versus conventional mitral valve surgery: prospective randomized study. Ann Thorac Surg. 2005;79(two):492–eight.
-
Sündermann SH, Czerny M, Falk V. Open vs. minimally invasive mitral valve surgery: surgical technique, indications and results. Cardiovasc Eng Technol. 2015;6(ii):160–6.
-
Svensson LG, Atik FA, Cosgrove DM, Blackstone EH, Rajeswaran J, Krishnaswamy G, et al. Minimally invasive versus conventional mitral valve surgery: a propensity-matched comparison. J Thorac Cardiovasc Surg. 2010;139(4):926–32.
-
Singh RG, Cappucci R, Kramer-Play a joke on R, Roman MJ, Kligfield P, Tapping JS, et al. Severe mitral regurgitation due to mitral valve prolapse: risk factors for evolution, progression, and need for mitral valve surgery. Am J Cardiol. 2000;85(2):193–eight.
-
Wilcken DE, Hickey AJ. Lifetime risk for patients with mitral valve prolapse of developing astringent valve regurgitation requiring surgery. Circulation. 1988;78(1):ten–iv.
-
Fukuda N, Oki T, Iuchi A, Tabata T, Manabe Chiliad, Kageji Y, et al. Predisposing factors for astringent mitral regurgitation in idiopathic mitral valve prolapse. Am J Cardiol. 1995;76(7):503–7.
-
Daneshmand MA, Milano CA, Rankin JS, Honeycutt EF, Swaminathan M, Shaw LK, et al. Mitral valve repair for degenerative affliction: a 20-year experience. Ann Thorac Surg. 2009;88(half dozen):1828–37.
-
Gammie JS, Sheng South, Griffith BP, Peterson ED, Rankin JS, O'Brien SM, et al. Trends in mitral valve surgery in the United States: results from the Society of Thoracic Surgeons adult cardiac surgery database. Ann Thorac Surg. 2009;87(five):1431–7.
-
Chikwe J, Toyoda D, Anyanwu A, et al. Relation of mitral valve surgery book to repair rate, durability, and survival. JACC. 2017;69:2397–409.
-
Bakaeen FG, Shroyer AL, Zenati MA, Badhwar V, Thourani VH, Gammie JS, et al. Mitral valve surgery in the US veterans assistants health arrangement: 10-year outcomes and trends. J Thorac Cardiovasc Surg. 2018;155(i):105–17.
Acknowledgments
We will like to give thanks the anesthesia section, the valvular centre disease clinic and the research department for the advisory and corrections for this manuscript.
Availability of data and materials
Database nerveless in the written report is bachelor from the corresponding author on reasonable request.
Data sharing is not applicable to this article every bit no datasets were generated or analyzed during the electric current study.
Author data
Affiliations
Contributions
JU, JC, NS, were the cardiac surgeons in charge of the patients. MG IP JU structured the commodity and wrote it. All authors read and approved the last manuscript.
Corresponding author
Ethics declarations
Ethics approving and consent to participate
The institutional review board waived blessing for this manuscript since the data was collected retrospectively and the follow up for patients either past phone or clinical visit is a regular procedure.
Institutional Review Lath: Comité de Ética en Investigación Clínica.
Consent for publication
Non applicative.
Competing interests
Dr. Juan P. Umana is a consultant for Edwards Lifesciences. Other authors declare that they accept no competing interests.
Publisher'south Annotation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed nether the terms of the Artistic Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you requite appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Eatables Public Domain Dedication waiver (http://creativecommons.org/publicdomain/nil/1.0/) applies to the data made available in this article, unless otherwise stated.
Reprints and Permissions
About this article
Cite this article
Giraldo-Grueso, M., Sandoval-Reyes, Due north., Camacho, J. et al. Mitral valve repair, how to make volume non matter; techniques, tendencies, and outcomes, a unmarried center feel. J Cardiothorac Surg thirteen, 108 (2018). https://doi.org/10.1186/s13019-018-0789-3
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s13019-018-0789-iii
Keywords
- Mitral regurgitation
- Mitral valve annulus repair
- Prolapsed mitral valve
Source: https://cardiothoracicsurgery.biomedcentral.com/articles/10.1186/s13019-018-0789-3
Posted by: alexanderanceent.blogspot.com


0 Response to "How To Repair A Mitral Valve"
Post a Comment